President Trump’s optimistic assessment that a coronavirus vaccine will be ready by the end of the year just got doused in cold water by a former top vaccine official.
Rick Bright, who directed the Biomedical Advanced Research and Development Authority until his removal last month, urged against rushing the process to develop a vaccine during his testimony before House Energy and Commerce Subcommittee on Health.
“A lot of optimism is swirling around a 12- to 18-month time frame, if everything goes perfectly,” Bright told lawmakers. “We’ve never seen everything go perfectly. My concern is that if we rush too quickly, and consider cutting out critical steps, we may not have a full assessment of the safety of that vaccine.”
Bright’s caution stood in stark contrast with a rosy prediction from Trump the same morning.
Shortly before Bright’s testimony yesterday, Trump said, “I think we’re going to have a vaccine by the end of the year.”
“We’re doing very well with the vaccine,” Trump told Maria Bartiromo in an interview on Fox Business. He suggested the military is being mobilized to help distribute a vaccine once it’s available.
“We’re of the assumption that by the end of the year we’re going to have a vaccine and then we have to be able to give it, to use it on most of our population,” he said.
Numerous experts, including Anthony S. Fauci, director of the National Institute of Allergy and Infectious Diseases, have said it could take between 12 and 18 months – at a minimum – to develop a vaccine.
Bright told lawmakers it normally takes up to a decade to make a vaccine. “We have done it faster in emergency situations … but for a novel virus, this has not been done yet that quickly.”
He added: “I still think 12 to 18 months is an aggressive schedule, and I think it’s going to take longer than that.”
Back in March, Fauci laid out a detailed timeline for vaccine development during testimony before the Senate Committee on Health, Education, Labor and Pensions. Fauci described a multistep process including clinical trials, trials that prove the vaccine candidates work and that they are safe for people to receive, saying the “entire process will take at least a year to a year and a half.”
During his latest testimony before lawmakers this week, Fauci referenced “at least eight candidate covid-19 vaccines in clinical development.”
Even as he said there was “no guarantee” about the effectiveness of a vaccine, he said he is “cautiously optimistic that we will, with one of the candidates, get an efficacy signal.”
Rick Bright, former director of the Biomedical Advanced Research and Development Authority, prepares to depart a House Energy and Commerce subcommittee hearing in Washington. (Greg Nash/Hill/Bloomberg News)
The Trump administration is racing to develop a coronavirus vaccine that could be distributed nationwide by January.
That’s what our colleagues Anne Gearan, Felicia Sonmez and Erica Werner reported late last month.
Health and Human Services Secretary Alex Azar referenced the project, dubbed “Operation Warp Speed,” as he jabbed at Bright and sought to undermine his Thursday testimony.
“While we’re launching Operation Warp Speed,” Azar said while standing next to Trump on the White House lawn, “he’s not showing up for work to be part of that.” In a statement, HHS questioned why Bright, who said he has been on medical leave with hypertension since his removal, hadn’t yet “shown up for work.”
Trump also dismissed Bright as an “angry, disgruntled employee.”
.@SecAzar: “On hydroxychloroquine, Dr. Bright literally signed the application for FDA authorization of it. Literally, he’s the sponsor of it.”
President Trump on Dr. Rick Bright: “He looks like an angry, disgruntled employee.” pic.twitter.com/IUnY6osr5y
— CSPAN (@cspan) May 14, 2020
Bright alleged in a whistleblower complaint filed earlier this month that he was pushed out of his role at BARDA in April and reassigned to a less prestigious role at the National Institutes of Health because he tried to “prioritize science and safety over political expediency” and raised concerns about a drug Trump touted as a possible coronavirus cure.
During his nearly four-hour-long testimony, Bright warned that the “window is closing to address this pandemic,” calling on the administration to develop a national testing strategy as well as a national plan for vaccine distribution. He cautioned against the government downplaying the possibility that it could take years to ready a vaccine for mass distribution.
Even if a vaccine is ready soon, Bright said the government has no plan in place for mass production.
“If you can imagine the scenario this fall or winter, maybe even early next spring, when a vaccine becomes available, there’s no one company that can produce enough for our country or for the world; it will be limited supplies,” Bright told lawmakers. “We need to have a strategy and plan in place now to make sure that we can not only fill that vaccine, make it, distribute it, but administer it in a fair and equitable plan.”
And supplies are not where they need to be, per Bright. He was asked about a BARDA estimate included in an addendum to his complaint that 650 million to 850 million needles and syringes would be needed to administer a vaccine nationwide, as well as an estimate from his BARDA team that it would take up to two years to manufacture these vaccine delivery supplies.
“It’s important to remember it’s not just the United States … when I said it would take two to two and a half years to make those, that was assuming there wouldn’t be global competition for those limited supplies,” he testified.

Dr. Rick Bright testifies before the House Energy and Commerce Subcommittee on Health on May 14, 2019, in Washington, DC. (Photo by GREG NASH/POOL/AFP via Getty Images)
The global grab over vaccines — let alone the necessary supplies to distribute them — could also be fierce.
If the coronavirus persists and becomes an endemic virus, our colleagues Christopher Rowland, Carolyn Y. Johnson and William Wan reported this week, public health experts worry the volume of available vaccine will fall short of demand. They fear a scenario where “manufacturers sell only to the highest bidders, rich countries try to buy up the supplies, and nations where manufacturers are located hoard vaccines for their own citizens.”
To that point, a French government official said yesterday it would be “unacceptable” to give the United States first access to a potential vaccine.
France’s secretary for economy and finance said it would be “unacceptable if there were privileged access from this or that country under a pretext that would be a monetary pretext,” pushing back on comments from Paul Hudson, the CEO of French pharmaceutical giant Sanofi, who said the “U.S. government has the right to the largest preorder because it’s invested in taking the risk.”
“There are more than 100 covid-19 vaccine research efforts in progress around the world, in laboratories in the United States, Britain, Germany, France and elsewhere,” our colleague James McAuley writes. “The question of national preference in these trials has been present from the beginning.”
Congress on coronavirus
Bright also testified that supply shortages and early inaction by the U.S. government cost lives.
He said he pushed for months to get increases in production of medical equipment, including masks — requests he said were ignored after he was told officials didn’t believe there was a “critical shortage.”
“I pushed that forward to the highest levels I could in HHS and got no response,” Bright said. “From that moment, I knew that we were going to have a crisis for our health-care workers because we were not taking action. We were already behind the ball. That was our last window of opportunity to turn on that production to save the lives of those health-care workers, and we didn’t act.”
In one exchange with Rep. Kathy Castor (D-Fla.), Bright described what he called an “absurd” response from HHS officials over his concerns about N95 shortages for front-line health workers.
“They indicated if we notice there is a shortage, that we will simply change the CDC guidelines to better inform people who should not be wearing those masks, so that would save those masks for our health-care workers,” Bright said. “My response was, ‘I cannot believe you can sit and say that with a straight face.’ That was absurd.”

President Trump and Health and Human Services Secretary Alex Azar. (Jabin Botsford/The Washington Post)
Officials within HHS reportedly were angered by Democratic lawmakers’ reliance on Bright’s testimony.
“For instance, Democrats on Thursday widely criticized HHS for declining to act on Bright’s urging to purchase masks from Mike Bowen, an executive at Texas-based Prestige Ameritech,” Politico’s Sarah Owermohle and Dan Diamond report. “But one current and one former official said that the administration eventually determined that the opportunity was not appropriate, adding that there was context missing from Bright’s testimony about why the U.S. government passed on the offer.”
They add: “Trump defenders were nowhere to be found in the House hearing room because they declined to send someone, giving Bright hours of air time and a news cycle’s worth of headlines.”
Ahh, oof and ouch
AHH: The Centers for Disease Control and Prevention is offering a brief set of guidelines to business, schools, day cares and others looking to begin reopening.
The documents are meant to help these facilities, which include restaurants, mass transit and camps, determine if they’re ready to open, and if so, the way to do so, a CDC spokesman told The Washington Post.

Checklists released by the CDC to guide schools, businesses and other organizations on reopening. (Jon Elswick/AP)
“The six checklists…come days, and in some cases weeks, after many states have begun to lift restrictions on their own. The advice is less detailed than draft recommendations the agency sent to the White House for review last month,” Lenny Bernstein, William Wan, Josh Dawsey and Holly Bailey report. “The nation is still awaiting that detailed technical guidance, which the White House has held up and not shared publicly. The delay has left the responsibility for decision-making about reopening to states and localities. It has also left many health experts clamoring for greater transparency.”
The White House had initially shelved the CDC guidelines, calling them “overly specific.”
The CDC said these six sets of recommendations were ready to go, so it released them while the other guidelines are pending review.
“In many ways, this advice is the only medicine we have,” Matthew Seeger, who has researched crisis communication for 35 years at Wayne State University, told The Post. “We don’t have a vaccine yet. We don’t have treatment. All we have is human behavior and that behavior is based on the information people get and whether they will listen to that information.”
OOF: White House officials have privately hinted they are open to providing tens of billions of dollars in relief to states.
The funding boost would be part of a bipartisan deal with Democrats that would come even as Trump has been reluctant to such funding, and as conservative groups remain strongly opposed, Robert Costa, Jeff Stein and Seung Min Kim report.

President Trump. (Alex Brandon/AP)
States have called for a massive influx of cash. This week, the National Governors Association repeated a call for $500 billion in aid.
“Although that position is likely to anger some Republicans who have warned that Democrats want ‘blue state bailouts,’ many White House officials now believe that providing new funding to states to deal with challenges related to the coronavirus pandemic will be necessary if they want to secure their own priorities, such as tax breaks and liability protections for businesses, the people said,” they write.
A pair of White House officials tell The Post they have told conservative allies and business leaders that the president isn’t “willing to provide a blank check” to states but is “open” to negotiating funding for states in exchange for concessions from Democrats on taxes.
OUCH: Small medical practices are particularly struggling.
Many are trying to stay afloat as their usual patients stay at home and postpone consultations, and as these practices fail to acquire federal loans under the Paycheck Protection Program, Rachel Weiner reports.
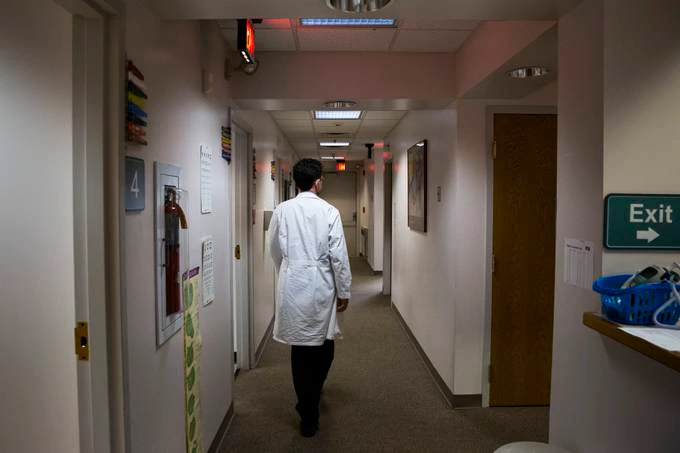
James Gill, president of Family Medicine at Greenhill, walks the halls of his practice in Wilmington, Del. (Rachel Wisniewski for The Washington Post)
“A survey done by a Richmond-based advocacy group for primary care doctors, called the Larry A. Green Center, found that half the doctors who sought such loans were unsuccessful,” she writes. “Of 2,774 doctors who responded to the survey, 19 percent said they had to temporarily close their practices because of financial problems; 42 percent had to lay off or furlough staff. About 10 percent say they will have to close in the next month because of financial shortfalls.”
Some doctors hope the ongoing pandemic could highlight a problem small practices have faced for years: high overhead and stagnant insurance reimbursement. Still, some fear they may not last long enough to see any changes in how they’re valued.
“Many physicians say their latest financial problems linked to the pandemic are only the most recent stress on a fast-vanishing model of health care in the United States as hospitals and large practices buy out independent doctors — often bringing higher costs,” Rachel writes.
Coronavirus latest
A few more stories to catch up on before the weekend:
The economic fallout:
- American small businesses and households, many with little in savings even before the pandemic, are quickly running out of money and struggling to pay their bills, Andrew Van Dam and Heather Long report.
- The prospects of a second round of stimulus checks for Americans are uncertain, even as the president has left the door open to the possibility, Erica Werner reports.
- About 3 million people filed for unemployment benefits last week, contributing to an eight-week total of 36.5 million workers who have sought to receive the benefits, Tony Romm reports.
The Trump administration’s response:
- Trump announced a plan to “replenish and modernize” the government’s undersupplied national stockpile of masks, ventilators and other essential medical equipment, Amy Goldstein reports.
In the states:
- Kentucky Gov. Andy Beshear (D) said he will lift the state’s travel ban next week. The order, which has been in place since March 30, prohibited travel out of the state and required people to self-quarantine for 14 days when entering the state, Steven Goff writes.
- Oregon Gov. Kate Brown (D) announced restaurants, bars and other businesses can begin reopening in 28 of the state’s 36 counties. “She rejected efforts by two counties that have experienced an increase in cases in the past two weeks, and three others continue to await approval,” Steven and Michael Brice-Saddler report. “Of the state’s 36 counties, the remaining three, which are around Portland — Clackamas, Multnomah and Washington — did not apply because of concerns about further outbreaks in the state’s most populous area.”