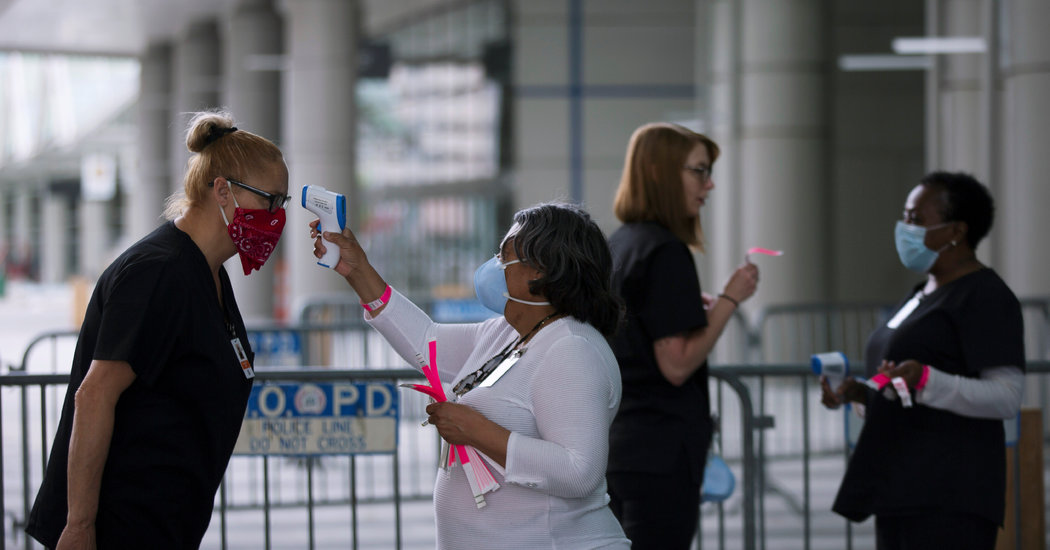In Louisiana, one of the states most devastated by the coronavirus, about 70 percent of the people who have died are African-American, officials announced on Monday, though only a third of the state’s population is black.
In the county around Milwaukee, where 27 percent of residents are black, nearly twice as many African-American residents tested positive for the virus as white people, figures released this week show.
And in Chicago, where African-American residents make up a little less than a third of the population, more than half of those found to have the virus are black. The death toll there is even more alarming: African-American residents make up 72 percent of those who have succumbed to the virus in Chicago.
“Those numbers take your breath away, they really do,” said Lori Lightfoot, the mayor of Chicago, who announced the city’s figures on Monday. “This is a call-to-action moment for all of us.”
Ms. Lightfoot, the first black woman to be elected mayor of the city, said in an interview that the statistics were “among the most shocking things I think I’ve seen as mayor.”
Data on the race of Americans who have been sickened by the coronavirus has only been made public in a handful of places, and it is too limited at this point, experts say, to make sweeping conclusions about the national or long-term picture. But day by day, the emerging statistics show black residents being infected at disturbing rates in some of the nation’s largest cities and states.
The racial disparities in coronavirus cases and outcomes, public health researchers said, reflect what happens when a viral pandemic is layered on top of entrenched inequalities.
The data emerging in some places, researchers said, is partly explained by factors that could make black Americans more vulnerable in any outbreak: They are less likely to be insured, more likely to have existing health conditions and, as a result of implicit racial bias, more likely to be denied testing and treatment. And then, the researchers said, there is the highly infectious nature of the coronavirus in a society where black Americans disproportionately hold jobs that do not allow them to stay at home.
“If you walk outside and see who is actually still working,” said Elaine Nsoesie, an infectious disease modeler at Boston University’s School of Public Health, “the data don’t seem surprising.”
States such as North Carolina and South Carolina have reported that, when compared with white residents, black residents account for a higher proportion of positive coronavirus tests than they represent in the general population. Black people are overrepresented compared with white people among those infected in the Las Vegas area and among those who have tested positive for the virus in Connecticut. In Minnesota, African-Americans have been infected with the coronavirus at rates roughly proportionate to their percentage of the state’s population.
Still, in many places, the data comes with a significant limitation. Officials are reporting racial data for cases where the patient’s race is known. For a large percentage of total cases in those places — sometimes more than 40 percent — no racial information is available.
And officials in many states, including those hard hit by the pandemic — California, New Jersey, New York and Washington — have not provided statewide information about the race of patients.
That has raised anger in some corners. Jumaane D. Williams, the public advocate for New York City, on Thursday sent a letter to Mayor Bill de Blasio calling for the release of a breakdown of cases by race. Senators Elizabeth Warren of Massachusetts, Kamala Harris of California and Cory Booker of New Jersey have demanded that the Trump administration collect race and ethnicity data on coronavirus testing and treatment.
“Despite the clear vulnerability of people of color in this public health emergency, comprehensive demographic data on the racial and ethnic characteristics of people who are tested or treated for Covid-19 does not exist,” the Democratic senators wrote in their letter, referring to the disease caused by the coronavirus.
As for the places where racial data has been tracked and made public, some experts pointed to longstanding structural inequalities as possible explanations for the disparities.
Sharrelle Barber, an assistant research professor of epidemiology and biostatistics at Drexel University, said government redlining policies that date to the 1930s left many neighborhoods with black residents lacking job opportunities, stable housing, grocery stores with healthy food and more. That has meant disproportionate rates of asthma and diabetes, she said, as well as residents who cannot simply stay inside their homes and away from work.
“These communities, structurally, they’re breeding grounds for the transmission of the disease,” she said. “It’s not biological. It’s really these existing structural inequalities that are going to shape the racial inequalities in this pandemic.”
Before the pandemic hit, officials had calculated that white Chicagoans had an average life expectancy of 8.8 years longer than black residents.
“Systemic and institutional racism that have driven these inequalities through the years we are now seeing play out in Covid data,” said Dr. Allison Arwady, director of the city’s public health department.
Officials on Monday said they would order health providers to offer complete demographic information on all coronavirus patients so Chicago could deploy what the mayor called “racial inequity rapid response teams” that would monitor symptoms, offer testing and help enforce social distancing in places like grocery stores. Plans were also being put in place to offer extra buses along busy routes so commuters could have more distance between one another.
In Detroit, the Rev. Larry Simmons said, “We see the same thing we always see: There’s a fundamental inequity in America, and this crisis of corona has just revealed it.”
Reporting was contributed by Audra D. S. Burch, Amy Harmon, Mitch Smith and Matt Furber.